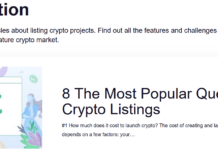
Rosacea is a skin disease that mainly occurs on the face: the skin on the nose, forehead, chin and cheeks turns red and clearly visible, dilated veins form. Depending on the severity of the rosacea, the skin will continue to bloom: pustules (purulent pimples) and papules (small, thickened nodules) will sprout.
Rosacea has other names that are now considered outdated or incorrect: acne rosacea, acne erythematosa, couperose or facial rose. Rosacea is also popularly known as copper rose, copper fin or red fin. Another common spelling is rosacea.
Rosacea is comparatively common. However, there are fluctuating data on the frequency of the skin disease. The Deutsche Rosacea Hilfe e.V. estimates that around four million adults in Germany are affected. The skin disease often develops in adults between the ages of 30 and 50. Children very rarely get rosacea.
Gender and skin type seem to play a role as risk factors for the skin disease rosacea. Women are about three times more likely to suffer from rosacea than men. However, men usually get sick more severely and get the skin disease a little later in life. Rosacea is also more common in fair-skinned people than in people with darker skin types.
Many believe that rosacea is contagious. However, this is not the case because the skin disease is not caused by bacteria or viruses. Rather, rosacea is one of the inflammatory skin diseases. In medical terms, rosacea corresponds to dermatitis (derma = skin, -itis = inflammation).
Rosacea is a chronic skin disease that comes in phases. A flare-up in which the disease is active and clearly visible is followed by symptom-free intervals. Dermatologists also differentiate between different degrees of severity of the disease.
Rosacea usually develops on the face, which some sufferers find emotionally distressing. First, the skin reddens and dilated veins form, which are clearly visible to the naked eye (similar to spider veins on the legs). Exactly these symptoms also occur with the skin disease couperose. Most dermatologists today assume that couperose is an early stage of rosacea. Doctors therefore call the early stage (stage 1) rosacea and not couperose. The early form of rosacea can continue to worsen and progress to more severe forms.
In addition to the reddening of the skin and the enlarged capillaries, pustules and nodules also form. Then the rosacea looks like acne. Except for the visual appearance, it has nothing in common with acne. The sebaceous glands and connective tissue can also proliferate in certain forms, causing the skin to thicken (phyme) – the typical bulbous nose sometimes forms, especially in men.
What helps with rosacea? What treatment makes rosacea go away forever? These are the most important questions for those affected, who often suffer from the disease. Doctors use various strategies to treat rosacea to improve the complexion.
Complete healing of rosacea is not yet possible, but the skin’s appearance can be significantly improved with the treatments.
Rosacea treatment aims to relieve the symptoms and psychological effects of the skin disease. Rosacea is visually noticeable because it mostly shows up on the face: Rosacea most commonly affects the nose, chin, forehead and cheeks. Yet only one in ten of the estimated four million people with rosacea see a doctor.
For many rosacea patients it is sufficient to only treat the skin externally (topical rosacea therapy). However, if the skin disease is more severe, doctors use additional drugs that work throughout the body (systemic treatment).
The following rosacea medications are approved for the treatment of the skin in Germany:
The following other remedies are sometimes used to treat rosacea, but are not approved for this purpose (“off-label use”):
Although some active ingredients are not approved for the clinical picture of rosacea, doctors still use them in some cases (“off-label use”).
In addition to the active ingredients used, the preparation of the medicines (gel, ointment, cream, emulsion) also plays an important role in terms of tolerability and effectiveness.
The skin of people with rosacea is usually particularly sensitive. The condition of the skin determines which means doctors choose to treat rosacea.
One problem with rosacea is that it often flares up again after people stop treatment. Dermatologists therefore recommend long-term therapy (maintenance therapy) in order to permanently improve the complexion. They usually use the active substance metronidazole for this purpose.
In the case of severe forms of rosacea, local treatment of the skin is often not sufficient. The same applies to mild forms of rosacea, where tried-and-tested medications no longer achieve sufficient success. Then doctors use tablets that work throughout the body (systemic therapy). Examples are:
When rosacea is severe, doctors always combine drugs that work locally on the skin with drugs that work throughout the body.
Dermatologists can also use laser treatment for rosacea therapy. The treatment is primarily an option when other treatment options have not been sufficiently successful.
It relieves skin redness, makes dilated capillaries disappear and refines the entire complexion. There are different laser techniques for the skin.
The IPL laser, for example, is effective against rosacea. The abbreviation IPL stands for “Intense Pulsed Light”. The laser emits controlled pulses of light, welds the blood vessels together and obliterates them – this reduces the reddening of the skin.
According to dermatologists, cosmetically good results can be achieved with IPL lasers – but also with other types of lasers (color lasers, diode lasers).
A treatment takes only a few minutes and is almost painless. Patients report that laser treatments feel like small pinpricks on the skin.
Several sessions are usually necessary and there is a risk that the skin symptoms will return after some time.
Anyone who has rosacea treated with a laser usually has to bear the costs themselves. Statutory health insurance companies usually do not pay for aesthetic therapies. There are better chances of having the costs covered by private health insurance companies. In any case, ask your insurance company beforehand.
However, many see cosmetic treatments as a good investment in their well-being. Discuss with your dermatologist how many sessions are necessary – depending on the severity – and how expensive the treatment will be overall.
Dermatologists know some triggers (so-called triggers) that promote rosacea. Sometimes they succeed in detecting these in a patient individually. Avoiding risk factors is considered the best home remedy for rosacea.
Spicy food, hot drinks or alcohol can promote the skin disease. Rosacea also increases with stress, which is why relaxation exercises in everyday life are also a good home remedy for rosacea.
Since the skin of people with rosacea is very sensitive, proper skin care is particularly important. However, home remedies can have different nourishing properties depending on the patient’s skin.
So try out what is good for your skin. It is important that you do not irritate your already stressed skin even more. And: home remedies and naturopathy alone are not suitable means to combat rosacea, but rather a supplement.
More home remedies for rosacea
Rosacea: does homeopathy help?
Some also try to treat their rosacea with homeopathy. However, there is no specific homeopathic remedy for rosacea. Homeopaths know some globules that are supposed to improve skin symptoms and refine the complexion. Examples are:
Even if rosacea cannot be cured, there are many treatment options to make the skin appear more beautiful.
The causes of rosacea and the mechanism of how the skin disease develops are still not clear. Researchers suspect that several factors are involved. According to current knowledge, there is no “one” cause of rosacea.
Doctors do not know of a rosacea virus, a fungus or a bacterium that causes the skin disease. However, germs of all kinds have an easy time on the attacked, irritated skin, penetrating through the damaged skin barrier and causing further inflammation.
It is likely that the innate, body’s defense mechanisms do not work as they should in patients with rosacea. For example, an intact immune system produces antimicrobial proteins to fight off germs on the skin, the so-called cathelicidins.
The skin produces these substances itself. They act like endogenous antibiotics, influence the immune system and promote the growth of blood vessels.
Researchers have found that cathelicidin production and activation is disrupted in people with rosacea. In patients, they detected many small cathelicidin fragments that are typical of rosacea and are not found in healthy skin. And these protein fragments in turn set inflammatory processes in motion.
The skin in rosacea reacts with inflammation. Hair follicle mites, so-called Demodex mites, are suspected to be the trigger. In fact, the skin of rosacea patients is much more densely populated with the mite Demodex folliculorum than the skin of healthy people.
The fact that therapies against the parasites also reduce the inflammation also speaks for the involvement of the mite in rosacea. An example of the active ingredients used in mite therapies is ivermectin, an antiparasitic.
Rosacea is almost always accompanied by reddening of the skin on the face that starts suddenly and in spasms. They often occur when a patient consumes spicy foods and alcohol or is exposed to an abrupt change in temperature. In some rosacea patients, measurements have actually shown increased blood circulation in the skin.
Researchers suspect that patients are hypersensitive to certain stimuli. The scientists discuss inflammation of the nerves and the influence of certain immune cells, the mast cells. There is a significantly increased number of mast cells in the skin of patients with rosacea.
Blood vessels, sensory nerves and mast cells lie close together in the skin and together regulate blood flow. The theory goes that if there are communication problems between those involved, the symptoms of rosacea could arise.
People with rosacea are more likely than other people to have an abnormal colonization of the small intestine, which doctors refer to as “small intestinal bacterial overgrowth”. The exact connection between this and the disease is not entirely clear.
In addition, doctors know some factors that can trigger flare-ups in rosacea. These include, for example:
The symptoms of rosacea appear mainly on the face, which is a psychological burden for some patients. Rosacea develops on the nose, forehead, chin and cheeks; there the skin suddenly turns red. Rosacea usually spares the region around the eyes.
The reddening of the skin can also affect areas near the face, such as the neck, neck, or back. This reddening of the skin is initially fleeting in the early stages and then disappears again. Later, however, it can persist for more than three months.
In addition, typical rosacea symptoms such as pustules (pimples), papules and dilated capillaries form. The latter can be seen with the naked eye and appear mainly on the cheeks.
In many patients, the skin itches, burns, and stings. Sometimes rosacea even spreads to the chest, back, neck, and scalp. Doctors divide rosacea into different degrees of severity depending on the severity.
The reddening of the skin, papules, pustules and dilated veins are particularly evident on the face. Facial care is therefore of central importance for rosacea. It is best to avoid using skin care products and cosmetics that further irritate the skin and increase symptoms.
For rosacea, only use facial care products whose composition is tailored to the specific needs of rosacea. Avoid chemical substances, such as those found in cosmetics, soaps and other skin care products.
People with rosacea are particularly sensitive to UV radiation. In addition, some patients take antibiotics (such as doxycycline) that make the skin more sensitive to sunlight. The result can be severe sunburn and skin damage.
Extreme temperatures fuel rosacea. Abrupt changes in temperature between cold and warm are considered to be an important trigger for rosacea. Protect your skin well if, for example, you do winter sports and then stay in overheated rooms.
The same applies to working in cold rooms and then moving to a warm office. If you use cold protection creams, it is best to remove them with a cloth when you go out into the warm – otherwise the heat builds up on the skin.
Covering, decorative foundation or make-up does not generally worsen rosacea. Red patches of skin are best concealed with green-tinted skin creams or make-up.
The products should be free from mineral oils, fragrances and preservatives. Points to remember: If you have applied any medicine to your skin, wait about 10 minutes. Only then do you apply the tinted skin cream or make-up.
Less suitable for rosacea are:
Dermatologists advise men with rosacea to shave dry instead of wet. After shaving, care for your skin with a balm that soothes the skin. Do not use disinfectant aftershave for facial care with rosacea – they irritate the skin.
Dermatologists differentiate between different degrees of severity in rosacea. The symptoms, the appearance and the severity of rosacea can vary greatly from person to person.
In the early stages of rosacea, fleeting, paroxysmal reddening of the skin occurs. Various external and internal stimuli can trigger this reddening of the skin.
These include, for example, irritating substances, spicy food, UV light or psychological stress. The skin is sensitive and very easily irritated. This fact unsettles some patients and sometimes also causes suffering.
In patients with rosacea stage 1, the reddening of the skin is permanent. In addition, enlarged veins form on the cheeks, which are differently pronounced. Many also report that their skin burns, stings, itches, is dry or flaky.
Typical of stage 2 rosacea is a permanent reddening of the skin that occurs on the nose, forehead, cheeks and chin. In addition, (usually symmetrical) inflamed, red papules and pustules form, which can persist for weeks. Sometimes accumulations of lymph fluid (lymphedema) develop that are easy to see and feel.
As the disease progresses, papulopustular rosacea can spread to the entire face. Even the chest, neck, cleavage and scalp can be affected. This degree of severity is similar to acne, but there are no blackheads.
With grade 3 rosacea, the connective tissue and the sebaceous glands proliferate: lumps (phymes) form, which are often found to be distressing by those affected. This form of rosacea primarily affects men. The growths grow on the nose (bulb nose), chin, jaw, forehead, ear, or eyelid.
In addition, doctors know some special forms of rosacea. These are:
Rosacea in babies or children is significantly less common than in adults. However, the appearance is very similar: papules, pustules, and dilated veins develop. In children, the eyes are often involved.
Sometimes the symptoms of rosacea even form first on the eyes and only then on the skin. The eyes are in the immediate vicinity of the frequently affected areas of the skin – it is therefore not uncommon for the inflammation to spread to each other.
Eye rosacea usually manifests itself in the form of eyelid inflammation and conjunctivitis. The symptoms are for example:
It is not uncommon for rosacea in babies or children to be more severe and with more complications than in adults, because the cornea of the eye can also be involved – which then threatens vision impairments. Doctors initially treat eyelid inflammation and conjunctivitis locally.
The following measures will help if your baby has rosacea of the eyes:
Doctors sometimes combine several of these treatments together. In addition, in some cases, they use antibiotics that are effective throughout the body.
Sources
This article was written by Ingrid Müller, biologist
The original of this post “Causes, treatment, care: everything you need to know about rosacea” comes from FOCUS doctor search.